Hygeia Note — A lively discussion has unfolded on GM_Ag focused on a novel COVID-19 drug therapy — inhaled budesonide, along with antibiotics and zinc. Many questions arose over the thin and anecdotal evidence suggesting that budesonide-based therapy is the magic COVID-19 cure sought the world over.
But the exchanges also yielded a compelling analysis by Michael Hansen of Consumer Reports explaining why Taiwan, Japan, and Singapore have been so successful in suppressing the virus — and without meaningful reliance on bedesonide. He also shares insights into why the U.S. has so tragically failed to contain the pandemic.
At the request of Hygeia Analytics, Michael prepared the below, lightly edited version of his budesonide GM-Ag post.
Over many years Michael has effectively represented Consumers Union in international food safety, regulatory, and public health meetings throughout Asia. These experiences provided him a nuanced understanding — and appreciation — of how Asian individuals and societies respond in the face of a pandemic. His insights harbor the seed of the path out of our nation’s ongoing COVID-19 nightmare.
Why and How Asian Countries Suppressed COVID-19
By: Michael Hansen, PhD
I question whether inhaled budesonide, along with antibiotics and zinc will cure COVID-19, and doubt that this treatment deserves credit for the low number of COVID-19 cases in Japan, Singapore and Taiwan, as some claim.
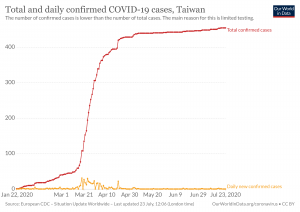 The example of Taiwan is instructive (see left). Some have argued that Taiwan has a population of some 24 million and that the island is not large enough to accommodate social distancing. So how has Taiwan kept COVID deaths so low (around a dozen) and confirmed cases to just a few hundred?
The example of Taiwan is instructive (see left). Some have argued that Taiwan has a population of some 24 million and that the island is not large enough to accommodate social distancing. So how has Taiwan kept COVID deaths so low (around a dozen) and confirmed cases to just a few hundred?
Taiwan has such a low number of cases and deaths because they took COVID-19 seriously very quickly. This is, in part, due to Taiwan’s experience with the 2003 SARS outbreak — another viral pathogen that came out of China. From its SARS experience, Taiwan did not have to be convinced of the importance of swift and strong preventive measures.
On December 31, 2019 after WHO made the announcement of cases of an unknown pneumonia in Wuhan, Taiwan officials started boarding airplanes arriving in Taiwan from Wuhan to screen passengers for COVID symptoms (fever, coughing). Any passengers showing signs of infection were tested and whenever possible, quarantined. More importantly, Taiwan immediately instituted a detailed plan of testing, isolation/containment of positives, and contact tracing.
Virtually everyone in Taiwan has a national health card with a unique ID that allows access to online treatment records. This health-identification system was effectively used to help in the fight against COVID-19. For people at high risk due to travel from Wuhan, their doctors were notified so that the individuals could be proactively tested, and quarantined if harboring the virus.
People with severe respiratory symptoms who had been tested for the flu were retested for SARS-CoV-2. Anyone that tested COVID-positive was quarantined at home, and GPS data from their phones was used to ensure that they remained in quarantine.
They also did contact tracing and close contacts were quarantined for 2 weeks. A study was published on the details and outcomes of contact tracing carried out in Taiwan in response to the first 100 confirmed COVID cases, including those dubbed close contacts. A “close contact” is defined as “a person who did not wear appropriate personal protection equipment (PPE) while having face-to-face contact with a confirmed case for more than 15 minutes during the investigation period.”
All identified close contacts were quarantined at home for 14 day, and tested if they showed any symptoms; there were 2,761 close contacts with 100 COVID-positive individuals — a remarkable average of nearly 28 people per infected individual.
The study was done between January 15 and March 18, and published on May 1 — an incredibly quick turnaround time. This research shows that Taiwan took this seriously and responded very rapidly with detailed data on their contact tracing and testing results. This paper’s findings also demonstrate that “high transmissibility of COVID-19 before and immediately after symptom onset suggests that finding and isolating symptomatic patients alone may not suffice to contain the epidemic.” A good review of the situation in Taiwan and the role that electronic health records played is accessible here.
Compare the situation of Taiwan with the US. Taiwan took the threat of COVID-19 seriously and immediately took detailed action to respond — test, contain/isolate, and contact trace.
The US, on the other hand, did almost nothing for months, has done virtually no contact tracing, and still has problems with testing, supplies of PPE, strained medical centers, and exhausted doctors and clinical staff.
Both Singapore and Japan have also taken quick action to identify cases, test them, isolate anyone that tests positive, or has been in contact with a known positive person. They have done rigorous contact tracing. Singapore and Taiwan both had bitter memories of the costs of SARS in 2003, so they were primed to take quick action when COVID arrived.

Also, mask wearing is a common and embraced response in all three countries, especially in the midst of a disease outbreak.
I am particularly impressed with the way that Taiwan was able to do detailed contact tracing. In the US, that is all but impossible. People here often do not comply with a simple request to name contacts. For example, a COVID-19 outbreak was linked to a big party just north of NYC where about 100 people attended and 9 tested positive, including the party host.
Having gatherings of more than 10 people is not legal in NY state, yet when authorities tried to get some of the positive individuals to reveal who else was at the party, they were met with silence. The local authorities had to issue subpoenas to compel them to reveal this information, losing time and the opportunity to nip spread in the bud.
There are also so many videos and stories about people refusing to wear masks and then threatening others, getting into fights, even shooting or stabbing people that ask them to wear masks in public. Just this week a man cursed at a police officer in Walmart when told he had to wear a mask, refused to give his driver’s license to the officer, and then hit the officer with his car before being arrested.
In fact in the US today, tragically, the simple act of wearing a mask in public is considered a political statement and those on the right, particularly avid supporters of President Trump, often refuse to wear masks, since this is considered a “violation” of their individual rights.
Far too many people believe that the pandemic is overblown, perhaps a hoax designed to hurt President Trump, or that masks don’t work and wearing one will make you sick. It has gotten so bad that a number of Republican governors have passed laws/regulations that forbid localities, such as Atlanta, from requiring people to wear masks in public, even when COVID-19 cases are skyrocketing and ICU beds are limited or only available — maybe, 600 miles away.
All of this is due, in large part, to the heavy strain of individualism that is part of the US character. This gene in our national fabric strongly contrasts with the more communal cultures in Japan, Taiwan and Singapore, where national and community considerations often override what individuals may want to do, and feel compelled to abide by.
In terms of the budesonide treatment, it should be pointed out that there is limited evidence of utility in treating COVID-19, particularly if inhaled. A study from Japan involving 3 older patients with COVID-19 pneumonia found that inhaled ciclesonide (a corticosteroid) had a strong positive effect, suggesting a possible treatment for COVID-19 pneumonia, but 3 is a very small sample size.
A review article on use of inhaled corticosteroids (ICS) concluded, “At present, there is no evidence as to whether pre-morbid use or continued administration of ICS is a factor for adverse or beneficial outcomes in acute respiratory infections due to coronavirus.” That said, there are some ongoing trials, such as one in England (the STOIC [Steroids in Covid-19] trial) which is recruiting almost 500 patients to determine if asthma inhalers (with budesonide) given to people with early emergency department presentations and hospital admissions will reduce infection.
Results from the RECOVERY trial, which involved 2,104 patients, demonstrated that dexamethasone (a corticosteroid), given either orally or by injection, reduced deaths by up to one-third in severely ill (those requiring ventilation) COVID-19 patients, and by 20% in patients needing oxygen, but not at all in patients that didn’t need oxygen or a ventilator.
The NIH is also looking into use of corticosteroids. Thus, while there is evidence that corticosteroids may provide benefits for treatment of COVID-19 patients with respiratory problems, we don’t know how useful it would be for treatment of COVID-19 cases with mild symptoms, but further research is clearly needed.
While there is evidence that corticosteroids, particularly ICS, may be useful for treatment of some COVID-19 cases, that’s a long way from saying budesonide is a magical, cheap cure for COVID-19. The reasons that Taiwan, Japan and Singapore have so few cases/deaths due to COVID-19, compared to the US, are generally known and accepted, and a flood of new research is now being published that reinforces the now-familiar, vital steps — testing, isolation of the infected, masks, social distancing, and contact tracing. The US did not take such actions. That’s the reason why cases in Taiwan, Singapore and Japan are so much lower than in US — not the fact that they are using ICS on a wide scale to treat COVID-19 cases.
I also have concerns about routine use of antibiotics in COVID therapy, especially in the absence of bacterial complications. A survey of COVID-19 patients treated at two hospitals in Wuhan found that while 95% (181/191) of the patients received antibiotics, only 15% (28/191) had secondary infections. A larger review of published studies of COVID-19 patients found that while 72% (1,450/2,010) were given antibiotics, only 8% (62/806) had bacterial or fungal co-infections. A doctor in Michigan noted that of more than 1,000 COVID-19 cases in Michigan, only 4% of those admitted to a hospital had bacterial co-infections, yet most patients were nonetheless given antibiotics soon after they arrived.
So clearly, there is a strong tendency to overuse antibiotics to treat COVID-19. In addition to the waste of money and valuable drugs, treating COVID patients with antibiotics may also impair an individual’s ability to naturally fight the virus, obviously not a welcomed side effect.
That’s my 2 cents.